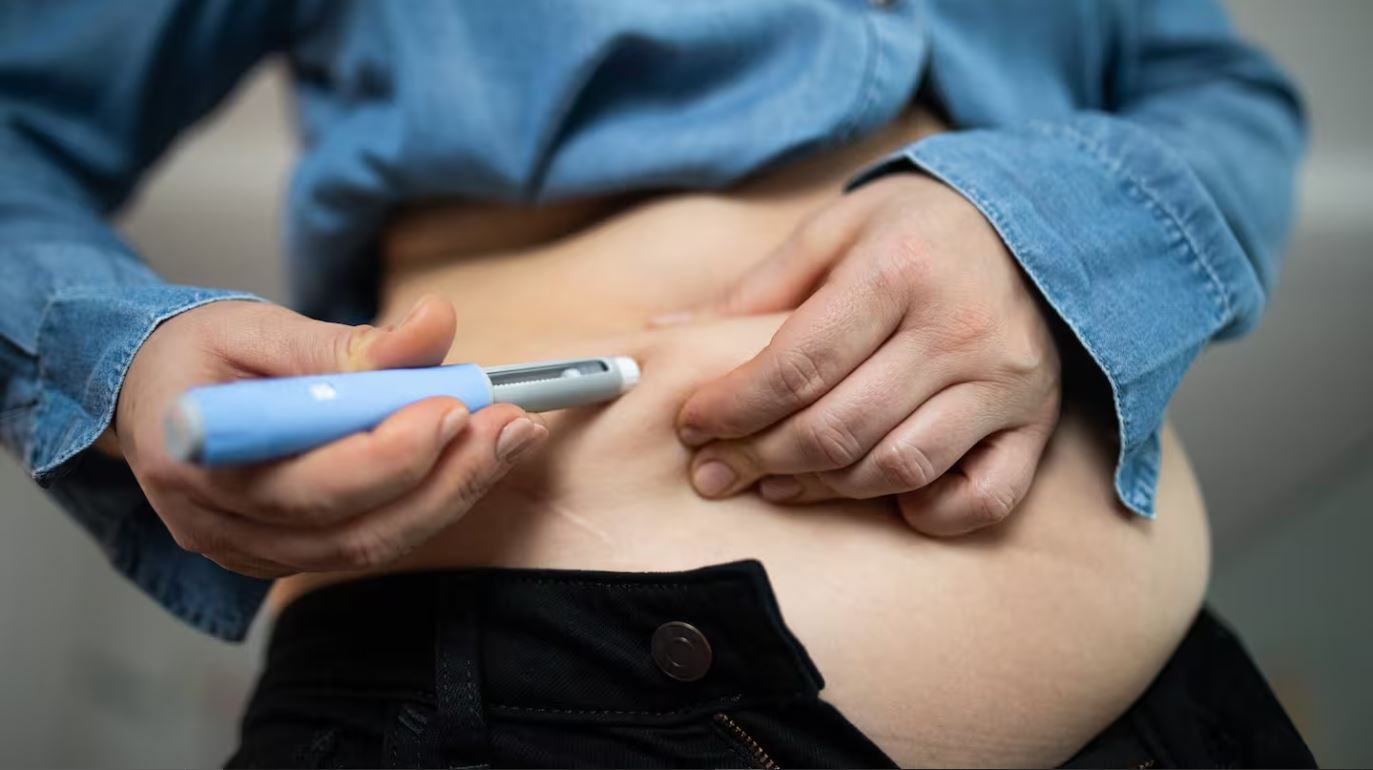
When Ozempic first made headlines as a diabetes drug that also caused dramatic weight loss, few scientists predicted where the research would lead. Today, GLP-1 receptor agonists, sold under brand names including Ozempic, Wegovy, Mounjaro, and Zepbound, are being investigated for more than a dozen conditions that have nothing to do with blood sugar. The science is still evolving, but the breadth of potential benefits is genuinely striking.
Their role is now being understood to be much more fundamental to human health, promoting longevity and preventing chronic illness progression, according to Muthiah Vaduganathan, a cardiologist at Brigham and Women's Hospital and faculty at Harvard Medical School. Here is a condition-by-condition breakdown of what the research actually shows.
What Are GLP-1 Receptor Agonists?
GLP-1 stands for glucagon-like peptide-1, a hormone your gut naturally releases after eating. It suppresses appetite and stimulates the release of insulin from the pancreas, which triggers glucose uptake from the blood. GLP-1 receptor agonist drugs mimic this hormone but last far longer in the body than the natural version, making them clinically useful for managing diabetes and obesity.
These medications are transforming the treatment landscape, dramatically improving the amount of weight loss achievable through medication alone or in combination with lifestyle interventions. In early clinical trials, patients on GLP-1 agonists achieved weight loss of 15 to 20 percent, compared to the 5 to 10 percent typically seen with previous medications, according to Miranda Stiewig-Rapp, assistant professor of endocrinology at UC Davis Health.
13 Surprising Benefits Researchers Are Discovering
1. Cardiovascular Protection Beyond Diabetes
This is perhaps the most well-established surprise. In 2024, semaglutide was approved by the FDA as the first weight-loss medication to reduce the risk of major adverse cardiovascular events in adults with obesity or who are overweight, without type 2 diabetes and established cardiovascular disease. The SELECT trial, involving over 17,000 patients, drove that approval. Semaglutide reduced the combined risk of heart attack, stroke, and cardiovascular death by roughly 20 percent compared to placebo.
2. Kidney Disease Progression
In January 2025, the FDA expanded the prescribing indications for semaglutide to reduce the risk of kidney disease progression, kidney failure, and death due to cardiovascular disease in adults with type 2 diabetes and chronic kidney disease. That decision followed a major trial showing a 24 percent relative risk reduction in kidney failure outcomes.
3. Heart Failure with Preserved Ejection Fraction
Researchers at Harvard Medical School found that GLP-1s were highly effective for patients with heart failure with preserved ejection fraction, a condition in which the heart muscle becomes so stiff that the ventricle holds less blood than usual, with a 40 percent improvement in key clinical outcomes. This form of heart failure has historically had very few effective treatment options.
4. Obstructive Sleep Apnea
In December 2024, the FDA made Zepbound the first approved treatment for moderate to severe obstructive sleep apnea in adults. Trials showed meaningful reductions in breathing interruptions per hour, likely driven by fat loss around the airway.
5. Fatty Liver Disease
Beyond weight loss, GLP-1 agonists have demonstrated the ability to combat fatty liver disease and alleviate obesity-related complications such as knee pain and acid reflux. Metabolic-associated steatohepatitis, the more severe form of fatty liver disease, is now a serious focus of ongoing clinical trials.
6. Osteoarthritis and Joint Pain
A study published in October 2024 in the New England Journal of Medicine found that patients in a randomized clinical trial who were treated with semaglutide had a meaningful decrease in pain from knee osteoarthritis and degenerative joint disorder. Researchers believe reduced mechanical load on joints and lower systemic inflammation both contribute to this effect.
7. Cognitive Decline and Dementia Risk
A paper published in January 2025 using U.S. Department of Veterans Affairs data of nearly 2.5 million patients found that people prescribed GLP-1 drugs had a lower relative risk of developing dementia compared with those who took other drugs for diabetes. A separate study found that liraglutide was tied to slower cognitive decline and appeared to reduce shrinkage in key regions of the brain. The EVOKE trials are now testing semaglutide directly in patients with early Alzheimer's disease, with results expected in 2026.
8. Stroke Risk Reduction
GLP-1 medicines reduce stroke incidence, as shown in major cardiovascular outcome trials including SELECT, SUSTAIN-6, REWIND, and PIONEER 6. These effects may result from metabolic improvements, direct actions in the central nervous system including modulation of neuroinflammation, reduced atherosclerosis, protection of vascular integrity, and reduced oxidative stress.
9. Alcohol Use Disorder and Addiction
A study published in February 2025 in JAMA Psychiatry found that patients with alcohol-use disorder drank less and had fewer cravings for alcohol and cigarettes over a nine-week treatment period when given a weekly injection of semaglutide. The mechanism involves the brain's reward circuitry. GLP-1 drugs blunt the dopamine response that normally makes calorie-dense food or addictive substances feel rewarding, according to UAB neuroscientist Andrew Hardaway. That same mechanism may apply to alcohol and other substances. There are now more than 15 clinical trials in progress globally examining GLP-1 agonists for substance use disorders involving tobacco, alcohol, and cocaine.
10. Depression and Anxiety
A large registry-based study found that people using GLP-1 medications had fewer psychiatric hospital visits and took less time off work due to mental health issues, with major drops in depression and anxiety observed among users. Researchers note that direct neurobiological mechanisms, including changes in the brain's reward system, may be involved alongside improvements in body image and glycemic control.
11. Inflammatory Diseases
A new frontier for GLP-1 drugs is chronic inflammation. Pharmaceutical researchers are now targeting what has been described as a broad category of inflammatory diseases, including Crohn's disease and severe skin and lung disorders. GLP-1 receptors are found in immune cells, and emerging data suggest these drugs may reduce the chronic, low-grade inflammation that underlies many modern diseases.
12. Gut Microbiome Shifts
GLP-1 therapies alter the way food moves through the gut and its fermentation patterns. These changes can shift the makeup of the microbiome, and a healthier microbiome in turn supports GLP-1 activity and improves insulin sensitivity. This bidirectional relationship between GLP-1 drugs and the gut microbiome is an active area of ongoing research.
13. Reward Pathway Rewiring and Compulsive Behavior
Beyond alcohol, researchers at UAB and other institutions are studying whether GLP-1 drugs influence compulsive behaviors more broadly. Scientists are investigating whether these drugs could help treat substance use disorders, which also involve dopamine-driven reward pathways. There are very few effective medications for substance use disorders, so there is significant excitement about whether this drug class could play a meaningful role.
Why Does One Drug Class Do So Much?
The breadth of effects is not accidental. Rather than addressing individual biomarkers linked to specific disease outcomes, GLP-1 drugs influence the central cardio-kidney metabolic process. Excess weight and adiposity are the fundamental drivers of why so many conditions are not only occurring but also progressing over time. Because GLP-1 receptor agonists target that root driver, they touch a wide range of connected diseases.
GLP-1 receptors are found in the heart, blood vessels, brain, kidneys, joints, and immune system. That anatomical distribution helps explain the diverse clinical signals researchers keep finding. Some benefits, including cardiovascular and renal protection, appear to occur partly independent of how much weight a patient actually loses, pointing to direct molecular effects at the receptor level.